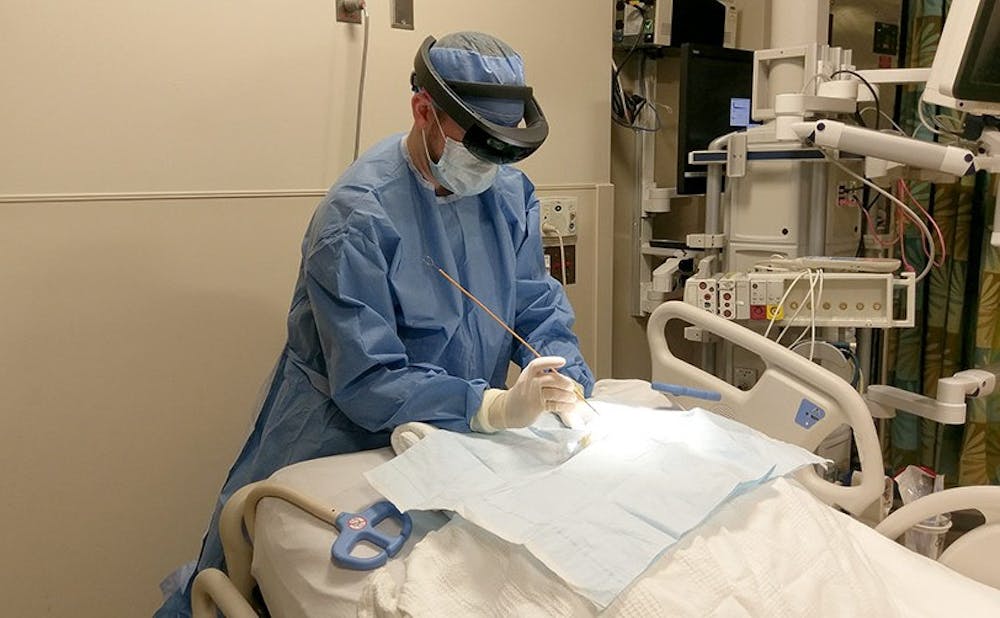
Neurosurgeons may soon be able to visualize hidden parts of the brain while performing surgery.
Neurosurgery residents Dr. Shervin Rahimpour and Dr. Andrew Cutler collaborated with Dr. Regis Kopper—director of Duke immersive Virtual Environment—and Yameng Liu, a master's student in engineering, to create a more efficient way to conduct brain procedures. Using a pair of augmented reality glasses known as Microsoft HoloLens, Kopper and Liu developed a simulation in which the ventricles in the brain were accurately overlaid on the head of a mannequin.
“Until HoloLens, [augmented reality] has been pretty unstable in the sense that it wasn’t very good at registering things in the environment in real time,” Kopper said.
Kopper added that although augmented and virtual reality are not entirely new to medicine, their use in the past has been limited.
“One of the early uses of [virtual reality] from the ‘90s was actually exposure therapy,” he said.
Exposure therapy is the psychological method of exposing patients to their fears in order to cure them. For example, a patient deathly afraid of heights may be repeatedly exposed to a cliff through virtual reality goggles to help overcome the fear.
But when Rahimpour and Cutler approached Kopper, they were interested in a far more complex simulation to help tackle a routine, yet occasionally tricky procedure—an extraventricular drain.
“What we all do emergently is drill a small hole in the skull and then pass this catheter into that fluid space to drain off the fluid,” Cutler said. “The idea is to drop the pressure immediately and give the fluid a new way to get out of the head.”
Although the surgery is typically routine, it can sometimes take a turn for the worse. Cutler explained that the traditional anatomical landmarks fail to work properly in certain situations, forcing the surgeon to guess how the catheter should be inserted.
With augmented reality, however, surgeons can avoid potentially dangerous guesswork.
“What this does uniquely is that it overlays the real environment with the virtual environment, so it helps you interact with both at the same time,” Rahimpour said.
In this case, neurosurgeons can visualize the ventricles in a patient’s brain on a Microsoft HoloLens screen based on a scan performed before the procedure.
The development process is still in its early phases, Kopper said. Although the concept of integrating augmented reality with surgery has proven feasible, the technology must improve before the device can be tested on anything other than a simple mannequin’s head.
“There’s some delay in tracking the catheter,” Cutler said. “Once that kind of picks up, we’ll be able to test it on models that we have, hopefully by the end of this academic year.”
Kopper added that other improvements could be made to the device.
“It’s still a bulky device, it’s heavy, but the main problem with the HoloLens is that the field of view is pretty small,” he said.
Even after these issues are ironed out, the implementation of augmented reality in medicine will continue.
“The procedure we have explored here is only the beginning,” wrote Dr. Patrick Codd, assistant professor of neurosurgery who advises Cutler and Rahimpour, in an email. “[Future improvements] could include making easily accessible, in real-time, multiple data streams including endoscopic video, patient vitals and patient MRI and CT imaging to the surgeon and the team throughout the operation."
Rahimpour explained that the simulation could also double as a training device for budding neurosurgeons, providing them with a safe way to practice newly learned operations.
Even though the project is still in its early stages, both the researchers and residents are optimistic about its potential.
“I’m excited for where the technology is going,” Cutler said. “I think as new generations of hardware and software come out, it’ll only get better and allow us to start jumping into other procedures and fields.”
Get The Chronicle straight to your inbox
Signup for our weekly newsletter. Cancel at any time.