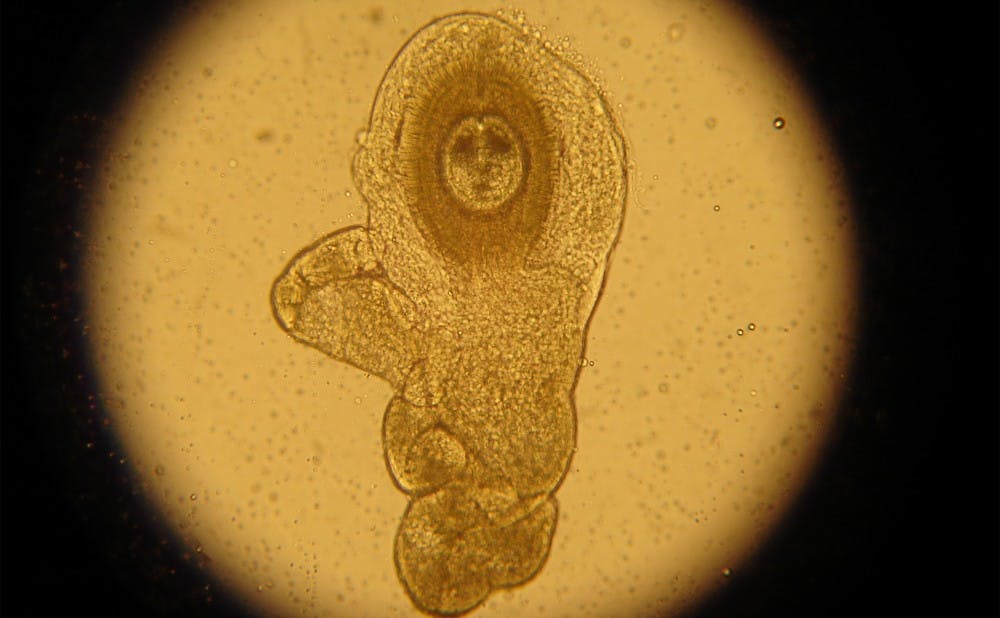
Eating intestinal worms may be a possible treatment for depression and other neurological diseases, according to a group of Duke scientists.
The research of William Parker, associate professor of surgery, and Staci Bilbo, associate professor of psychology and neuroscience, indicates that certain organisms, like intestinal worms called helminths, can exist inside the human body in a mutually beneficial relationship with bacteria in the gut. Parker and Bilbo argue that modern society’s efforts to remove organisms such as helminths has resulted in increased rates of autoimmune diseases such as allergies.
Helminthic therapy is an effort to rebalance the immune system and address a variety of disorders by putting the helminth worms back into the human body. Although the Food and Drug Administration has not currently approved helminths as a treatment method, some people have begun to treat themselves using the organisms and have reported positive effects.
Parker and his colleagues are currently planning a clinical trial to investigate whether helminths could treat depression.
“The goal here at Duke is to get helminths approved by the FDA so we can begin clinical trials,” Bilbo said. “The first target is depression because the condition is thought, at least for a significant subset of people, to involve the immune system having a pro-inflammatory signature, so the idea is, treat your gut and heal your brain.”
These efforts have been prompted by reports from people who ingested commercially brought helminths to treat their own disorders, ranging from depression to allergies. Parker worked with Duke undergraduates to collect information about these self-treaters. The students interviewed providers, surveyed the web and sent out surveys.
“The effectiveness of the helminths is substantially better from whatever effect they were getting from pharmaceutical treatments and the side effects are much less. It’s a pretty profound difference,” Parker said.
Parker also reached out to Bilbo, a neuroimmunologist, and her research provided evidence that helminths can effectively prevent autoimmune reactions—which involve the immune system attacking healthy cells—in mice.
“The number one job of helminths is to prevent [themselves] from being detected and expelled by our immune system, so they secrete all kinds of anti-inflammatory factors that calm the immune system,” Bilbo explained.
Her studies with mice have demonstrated that the worms can prevent hypersensitive immune responses that affect the brain without compromising their immune systems. They also suggest that helminthic therapy in humans could be promising, although the beneficial effects could vary from individual to individual, Bilbo said.
Mental health conditions like depression are among the hardest disorders to clinically treat, making helminthic therapy a better alternative to current drugs in the market, she added.
“Now we don’t think everyone is going to benefit but if we can treat 25 to 30 percent of people with treatment-resistant depression, it would be huge, and it will be extremely inexpensive and simple,” she said. “Just once a month you swallow a few of these larvae and that’s it.”
In order for human helminthic therapy to be a scientifically sound and accepted treatment, Parker and his colleagues need empirical evidence from clinical trials. Parker and Bilbo are currently applying for FDA approval for clinical trials involving helminths.
In the long run, Parker hopes that helminths will become an inexpensive way of balancing immune function.
“In every aspect, it is much like a vitamin—it is an important part of the ecosystem of our body that we can’t live without,” he said.
Get The Chronicle straight to your inbox
Signup for our weekly newsletter. Cancel at any time.